A nurse-led satellite clinic initiative for STI testing in an Australian correctional center: a qualitative study
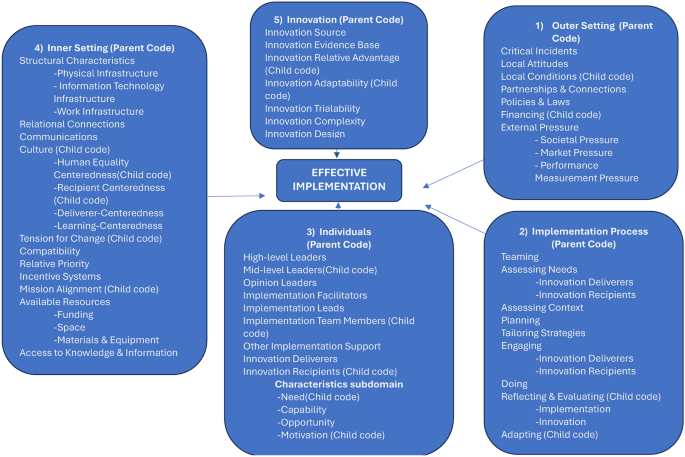
Outer setting domain
The overarching theme for the outer setting domain related to ‘Meeting the needs of incarcerated people’. The needs identified by both incarcerated people and satellite STI clinic nurses highlighted that incarcerated people both want and need sexual health education. To meet this need and recommendation, additional funding is required by offering further STI testing through the week, coupled with sexual health education, with more staff engaged in the STI testing, treatment and prevention. Limited access to health services both within and outside the carceral setting was a barrier to incarcerated people receiving testing, treatment, and prevention through sexual health education. This issue is compounded with the low level of health literacy among the carceral population, including difficulties understanding health promotion messaging due to poor reading skills (see Table 2). A study by Tenibiaje et al. considered the literacy and health literacy levels among incarcerated adults in Nigerian prisons which were both found to be deficient within this cohort39. This study highlighted the significant impact low levels of literacy have on health literacy which in turn has a deteremental effect on the health and wellbeing of incarcerated populations39.
Satellite STI clinic nurses identified how taking the STI testing, and sexual health education to the incarcerated population in their accommodation setting, resulted in increased number of incarcerated people being tested, treated, and educated (see Table 2). This positive outcome was rooted in improved access. Findings from this study parallels with that of Pimenta et al.’s study focusing on opportunistic testing for chlamydia in both primary and secondary healthcare environments and the positive associations this may have40. Although access to testing was not a factor in Pimenta et al.’s study, testing asymptomatic patients opportunistically no matter their initial reason for attending the healthcare facility, was found to be both acceptable, and a suitable method for upscale40.
Recommendations
The need for additional funding and education related to sexual health for incarcerated people
A key recommendation relates to the continued funding for the satellite STI clinic to maximize continued fruitful uptake, and for the upscale of the satellite STI clinics nation-wide. It is recommended that the additional funding be allocated to the improvement and expansion of the sexual health education component of this satellite STI clinic to better align with WHO’s recommendations to provide comprehensive sexuality education, including STIs and HIV, and adequate health service interventions for vulnerable populations, such as incarcerated people1.
Implementation process domain
The overarching theme for the implementation process domain was ‘Adaption based on need.’ This theme was strongly focused on listening to feedback, responding to the needs of incarcerated people and satellite STI clinical nurses, and adapting the process if required. Whilst one incarcerated participant requested ‘More confidentiality, NO prison Corrections Officer’ (see Table 2) this is an inactionable request as nursing staff are, due to safety precautions, required to be accompanied by prison officers when conducting clinics.
Similarly, to the authors’ knowledge, satellite clinics providing mobile medical care within carceral settings is an under-researched area. However, studies involving mobile STI testing clinics within the community have, similar to the current study, had positive outcomes in relation to improving testing and treatment for the targeted population41. For example, a study by Heese et al. focused on mobile STI testing within the community found that taking STI testing to/near to populations vulnerable to contracting STIs, improved accessibility and uptake41. As such and for future upscale, the authors of this article recommend the STI clinics remain satellite to reduce the burden on medical centers, to improve workflow, and importantly, increase access and uptake to STI testing, treatment and prevention through sexual health education. Parallel to this, both incarcerated people and satellite STI clinic nurses highlighted that high risk STI-inducing behaviors were undertaken in the carceral setting (see Table 2), offering valuable insights into how and why some STIs are spreading in real time. This information would further enhance the sexual health education to be adapted to be further relevant and meet the needs of the incarcerated population.
Recommendations
Having appropriately skilled nursing staff running the clinics
Future staffing considerations should include nurses who are approachable, non-judgmental, knowledgeable, and capable of building therapeutic working relationships with incarcerated people. Whilst the lead author intends to upscale the satellite STI testing program with the sexual health team currently in place, the inclusion of an increased staffing pool to implement the clinic at each center during upscale is imperative for its success. Open-ended satisfaction survey responses need to be monitored to ensure incarcerated people’s high satisfaction with the nurses delivering the satellite STI clinic continues.
Individuals domain
The overarching theme for the Individuals domain was ‘Nursing staff motivation’, and the ‘Incarcerated population’s desire to be healthy.’ One barrier relating to gaining approval for the WUG process, was associated with the extensive time satellite STI clinic nurses were spending applying for and gaining WUG approval (see Table 2). A study by McFadyen and Rankin identified that research involving vulnerable populations, often have gatekeepers outside the ethics approval process who may contribute additional barriers for researchers42. Apa et al.’s study exploring the challenges and strategies to conduct research in prisons had similar findings, highlighting the additional barriers to obtaining appropriate permissions when conducting research with incarcerated people, including the additional time required to review protocols for implementation43. When developing a collaborate research relationship Apa et al., stress how establishing prison contacts, and maintaining rigorous research methods are key to successfully conducting research with incarcerated populations43. In applying this learning, and to overcome the barriers experienced in this study, future practice would benefit from including the development of a statewide carceral implementation toolkit. Once approved, this toolkit could be applied to carceral environments negating the need for multiple applications, expediating the implementation of the satellite STI testing clinic. As reported in research, evidence-informed toolkits are used to facilitate the implementation of evidence-based interventions by providing resources that are adaptable and customizable, in turn accelerating the process of translating research into practice44.
A large cohort of the incarcerated people also requested, through the open-ended survey questions, access to prophylaxis such as condoms (see Table 2). Currently, accessing these items through diverse STI and BBV preventative programs are unavailable to people incarcerated in Queensland35. Yet some programs in correctional centers in other Australian jurisdictions offer access to condoms (and dental dams) through vending machines, such as NSW, VIC, Western Australia, and Tasmania12.
Recommendations
Collaboration with policy makers
It is recommended that policy makers work with correctional services to consider the implementation of a condom/dental dam distribution, for incarcerated populations within the next six months to ensure alignment with WHO recommendations7 and incarnated people’s right to ‘the enjoyment of the highest attainable standard of physical and mental health’31. Additionally, these policy makers could work to incorporate this as ‘core business’ within state and national strategies with a large scale evaluation, including health economic evaluation for future research within the same timeframe.
Inner setting domain
The overarching theme within the inner setting domain was ‘Shared vision’ based on the high levels of support of implementing the satellite STI testing clinic evident both from the incarcerated peoples’ open-ended survey responses, and the responses from satellite STI clinic nurses (see Table 2). Scholars have identified that successful integration of EBP require support from both the researchers implementing the intervention, and from diverse stakeholders within the organization/setting38,45. Within this context, the satellite STI clinic nurses identified that the satellite STI testing program received overwhelming support from all levels within Queensland Health, and that of QCS (see Table 2). At each level of the organizations a shared vision was present, in turn playing a contributing factor to the clinic’s success.
Recommendations
Continued intraorganizational cooperation, and the continued adaptability of the program
It is recommended that for upscale of this satellite STI testing program, further communication, co-operation and input from all levels within Queensland Health and QCS be maintained. It is also recommended that the satellite STI clinics continue to be adapted, where and when required, considering stakeholder input at all levels. With continued senior level support, being embedded in policy, and not susceptible to changes to staffing and/or changes to ruling political parties, this program has a greater chance to continue and thrive.
Successful implementation of this recommendation will be evidenced by a continuation of open communication pathways, intraorganizational cooperation, and adaptability of the satellite STI clinic program. It is also recommended that this model, due to its adaptability, be embedded into all quality improvement activities, to enhance EBP within correctional settings, and to enhance clinically relevant research culture. This model can also be adapted to each specific future carceral site to enhance relevance and feasibility.
Innovation domain
The overarching theme for the innovation domain related to the ‘Efficacy of clinics due to the ‘satellite method’. This was strongly supported by the incarcerated participants and the satellite STI clinic nurses, with both expressing the effectiveness of the satellite STI clinic method, and the need for additional days to run the clinics (see Table 2). This need also considered the delays deriving from the pathology section of the carceral setting needing to send the pathology specimen to the local hospital, and the needs of the incarcerated people to have a quick turnaround from testing to treatment, especially if an individual tested positive. Advertising of future satellite STI clinics was also asked for, and a small number of incarcerated people requested that STI testing also be made available in the medical center (see Table 2).
Recommendations
Additional days, advertising, and modes of delivery
It is recommended that for the upscale of this project, satellite STI testing clinics should be delivered and offered additional days per week based on the demand outstripping the current and available financial resources. Similarly, the clinics will need to be announced and advertised in advance to provide adequate awareness that the nurses will be attending, and when. Finally, it is recommended that testing be offered in the medical center as an additional service securing accessibility. These recommendations should be implemented within the study site, and as a core component regarding the upscale of the clinics. To evaluate the success of these recommendations, additional closed and open-ended satisfaction survey questions can be included for the incarcerated population.
Strengths and limitations
This study had multiple strengths, including the innovative nature of the study and the high level of uptake and acceptance, in turn demonstrating the need for clinic upscale. A key strength of the study was the innovative delivery of the satellite method to overcomes barriers that are impeding on incarcerated people from accessing STI testing, treatment and prevention within the carceral environment. This was evidenced by the nursing staff motivation, shared vision, and the incarcerated persons’ desire to be healthy. The clinics were well-received with engagement from multiple stakeholders, including multiple levels within Queensland Health, and QCS. This study has the potential for upscaling and promoting STI testing, treatment and prevention through sexual health education, collectively contributing to EBP and having real-world translational impact. Through EBP, this nurse-led sexual health clinic meets the needs of incarcerated people, by providing access to sexual health services, in an environment, typically known for challenging access these services. As such, this well-utilized and accepted model could be applied to other health care interventions focused on improving access to care for incarcerated people.
There were multiple limitations to this study including significant time delays associated with data collection due to multiple external research approval processes. Another limitation was the brevity of qualitative feedback from both the incarcerated population and from the satellite STI clinic nurses. It is recommended that in-depth interviews are conducted with future participants to gain greater insights regarding barriers/facilitators associated with the satellite STI clinic to inform future quality improvements, and adaptations of the program to meet the needs of incarcerated people.
A further limitation concerned the demands for the clinic outweighing the service delivery where funding allocated to run the clinic provided limited staffing and hours. Additional staffing and availability of hours would provide a better understanding of potential demand/uptake for the satellite STI clinic. However, initial findings are promising and warrant continuation of this service with room for adaption and to be replicated in further correctional settings in Australia, including globally.
As this study was within one correctional site in Queensland, Australia, caution must be used regarding generalizability of findings to other correctional facilities, including those outside of Queensland and Australia. However, the initial findings from this exploratory study provide the potential for further widescale implementation and evaluation.
Similarly, the potential needs of diverse sub-groups within the incarcerated cohort were unknown due the brevity of questions in the satisfaction survey, and those choosing to not engage with the pilot clinic and/or not completing the evaluation component of the satellite STI testing clinic. Likewise, although incarcerated transgender women residing in the facility were invited to utilize the satellite STI testing clinic, data related to the gender of the participants was not collected. As such, no unique data were collected concerning the transgender women who may have engaged in the service. The demographic data collected included sex assigned at birth but neglected to collect data surrounding the gender the participants identified with. Brömdal et al., highlight that transgender women within carceral setting are more susceptible to sexual violence, lack sexual health knowledge, and have reduced access to sexual health services, collectively increasing their vulnerability to contract STIs46. This oversight translated to valuable data from a vulnerable and at-risk sub-group within the carceral setting was not considered.
This study adapted Lam et al.’s CFIR guided semi-structured interview questions, which presented to be a feasible and replicable semi-structured interviewing framework and can be applied to multiple different research environments23. In applying these semi-structured interview questions to this study, we were able to conduct an evaluation of the constructs for the effective implementation of the satellite STI testing clinic based on the nurses’ feedback. However, one limitation in utilizing this framework was the potential for unintentionally excluding themes that did not fit within the CFIR construct. The potential omission of themes was also highlighted within Lam et al.’s evaluation of the farmwork as a potential limitation23. This limitation therefore also applies to our use of deductive analysis where the strict adherence to pre-existing objectives47, such as our research question, and codes applied from the CFIR framework meant that important underlying themes that did not fit within these constructs may have been overlooked.
link






