Emerging burden of post-cancer therapy complications on unplanned hospitalisation and costs among Australian cancer patients: a retrospective cohort study over 14 years
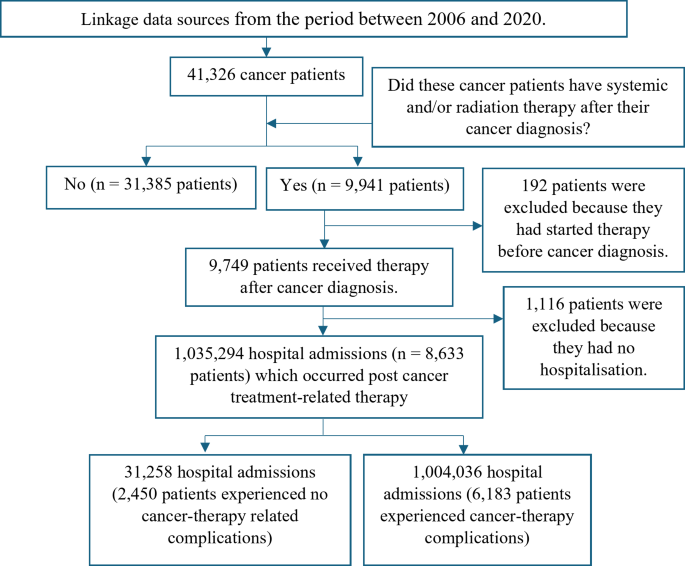
This study provides a comprehensive analysis of post-therapy complications among cancer patients, highlighting significant increases in hospitalisation length of stay (LOS) and medical costs. Notably, 72% of patients developed complications post-systemic and/or radiation therapy, predominantly manifesting as anemia, sepsis, nausea and vomiting, and neutropenia. The types of cancer most frequently associated with these complications were acute lymphoblastic leukemia, multiple myeloma, melanoma, kidney, Hodgkin lymphoma, esophageal cancer, non-Hodgkin lymphoma, and stomach among the participants. Patients experiencing post-therapy complications had an average increase in hospital LOS by 1.72 additional days, reflecting unplanned extensions beyond their initial treatment plans. These patients also faced significantly higher hospitalisation costs, with additional expenses averaging AU$8,791 compared to those without complications.
Our analysis revealed that patients who underwent both systemic therapy and radiotherapy had an 8.24 times higher chance of experiencing post-therapy complications compared with those who only received systemic therapy. These findings are consistent with previous studies that also showed a correlation between receiving cancer therapies and post-therapy complications34,36,37. This increased risk might be attributable to the cumulative toxic effects of multiple therapies on patient health, as suggested in other studies34,36,37. This comparative insight is crucial for healthcare providers in strategising care to mitigate these risks, particularly in treatments involving multiple therapy modalities38.
This study highlighted the significance of post-therapy and revealed that patients who experienced complications, such as prolonged following therapy, had significantly longer unplanned hospital stays and compared with those who did not experience any complications. This finding is consistent with published data that indicates patients with post-therapeutic complications have longer hospital stays and higher treatment costs12,14,18,19,39. These results reinforce the critical need for effective monitoring and management of patients during and after cancer treatment to mitigate the risks associated with post-therapy complications. Such complications not only impose a substantial economic burden on patients and the healthcare system but also potentially delay ongoing cancer treatment40, adversely affecting patient outcomes. It is imperative that healthcare providers implement robust strategies for early identification and management of potential complications. Assessing factors such as performance status, organ function, comorbidity, and patient frailty can guide clinicians in tailoring treatment plans that minimise the risk of adverse effects18,34,41. Moreover, proper communication with patients about the potential for hospitalisations and other treatment-related adverse events is essential. Providing detailed information helps patients make informed decisions about their treatment options, balancing the benefits against the risks. This approach can significantly improve the quality of care, reduce the impact on healthcare resources, and enhance the overall quality of life for patients and their caregivers.
Treatment-related complications, including anemia, sepsis, and neutropenia that occur after systemic and radiotherapy, have been found to be associated with longer hospitalisation stay per admission. Cancer patients undergoing active treatment are often immunocompromised, which makes them more susceptible to sepsis leading to mortality. Previous studies show that cancer patients have a higher incidence of severe sepsis, which results in increased hospitalisation and mortality14,18. For example, cancer patients with severe sepsis stayed in hospital for almost three times as long as cancer patients without severe sepsis14,18. Anemia is also prevalent among cancer patients and can lead to longer hospitalisation in the oncology unit31,42. These occurrences can adversely impact overall survivorship, quality of life, and increase length of hospital stay43. Neutropenia is another severe complication of chemotherapy among cancer patients. Patients who experience neutropenia mostly have longer hospitalisation periods44. Another study found that neutropenia is a life-threatening toxic effect of chemotherapy that can be responsible for longer hospital LOS39. However, the toxicity profile of each cancer treatment modality varies according to dosages, treatment duration, and patient characteristics. These findings highlight the need to manage these complications effectively with supportive measures at home or by increasing outpatient monitoring. Furthermore, it underlines the importance of preventing hospitalisation due to therapy-related complications to optimise patient outcomes. While the reasons for prolonged LOS without complications were not directly examined in this study. However, previous studies indicated that factors including pain, infection and dyspnea can influence hospitalisation14,24,31,41,45.
Study strengths and limitations
The main strength of this study was the use of a large cohort of cancer patients from Victoria, Australia. Data was extracted from administrative linked data sources, including the Victorian Admitted Episodes Dataset, for the period between 2006 and 2020. These administrative datasets are based on hospital data compiled by individual public and private hospitals through two hospital networks in Victoria, Australia. This study conducted a 14-year longitudinal analysis among medically diagnosed cancer patients, allowing the identification of trends and changes in the burden of post-therapy complications over time. By capturing associations, this analysis aids in understanding how therapy practices and patient health outcomes have evolved. It is important to note that while this study identifies associations, it does not establish causality between treatment practices and patient outcomes. This study adopted a comprehensive approach by investigating complications from several aspects, including clinical characteristics, hospitalisation, and healthcare system costs from the Australian healthcare system perspective. This multifaceted exploration improves the understanding of the complexities surrounding post-therapy complications.
This study has some limitations such as data was collected from only two hospital networks in metropolitan Victoria. However, it is important to note that the results may not be fully representative of the entire state and might be biased towards a particular population. To ensure accurate and reliable results, a more comprehensive study would be required, which would involve collecting data from a state-wide cancer registry and including data from all state hospitals. By doing so, we can ensure that our findings are based on extensive and diverse data, and that we can make confident and reliable conclusions. The study was conducted from the Australian healthcare system perspective and assessed the direct medical costs of unplanned hospitalisation due to post-therapy complications in cancer patients. However, patients who experience post-therapy complications may also incur greater indirect costs, such as psychological stress, reduced productivity in daily activities, and increased time off from work and additional care burdens on their family members. In order to perform rigorous explorations for the economic analysis of post-therapy complications, healthcare utilisation data, including Medicare claims through the Medicare Benefits Schedule (MBS) and Pharmaceutical Benefits Schedule (PBS) claims data, is required. Unfortunately, we were unable to capture all aspects of healthcare use and assess the long-term economic impact of these cancer patients due to a lack of data access and funding. The substantial group size imbalance, with the majority of patients receiving systemic therapy only, may have impacted the precision of estimates, and this limitation should be considered when interpreting the findings. We acknowledge that the stages of cancer among patients may significantly influence the choice of treatment modalities and subsequent risk of complications, which may not be fully captured by the analysis of this specific subgroup within our study. Moreover, the study considered post-therapy complications according to the study design and research questions, while cancer patients may also be diagnosed with non-cancer chronic comorbid conditions or diseases, which may contribute to a higher disease burden and hospitalisation events. However, we acknowledge that the inclusion of performance status, comorbidity indices, frailty, and organ function could enrich the analysis, providing a more nuanced understanding of risk factors associated with post-therapy complications and their economic impact. The absence of these variables in our analysis is indeed a limitation, as it could affect the depth of risk stratification and potentially influence the interpretation of our findings. Therefore, future research is required using a similar study design that captures all relevant aspects of healthcare use in an economic assessment to provide robust evidence for policymakers and stakeholders. In addition, we recommend that future clinical studies with larger subsets of patients receiving combined therapies be conducted to validate and expand upon these findings.
Implications and key recommendations
The research findings have several policy implications for the Australian healthcare system, addressing various aspects of cancer care and post-therapy complications. This study proposes some key recommendations:
-
(1)
Develop risk stratification models to accurately identify patients at a higher risk of post-therapy complications. This should focus on factors such as age, gender, health conditions, and specific cancer types. Implement targeted interventions for these high-risk groups to ensure early detection, monitoring, and effective management of complications.
-
(2)
Given the observed higher risk of complications among patients receiving both systemic therapy and radiotherapy—despite the small size of this subgroup—, it is prudent to advocate, for a more cautious approach. We recommend the implication of tailored treatment protocols for these patients, which include enhanced monitoring and coordinated care. These protocols should focus on active surveillance, early detection, and prompt management of potential complications. This approach may help mitigate the risks associated with combined treatment modalities and improve patient outcomes.
-
(3)
Establish strategies for continuous monitoring and enhancement of the quality of cancer care. Consistently assess the occurrence of post-therapy complications, evaluate the impact on hospitalisation, and adjust healthcare practices accordingly. This could involve regular assessments and incorporating lessons learned into clinical guidelines.
link






